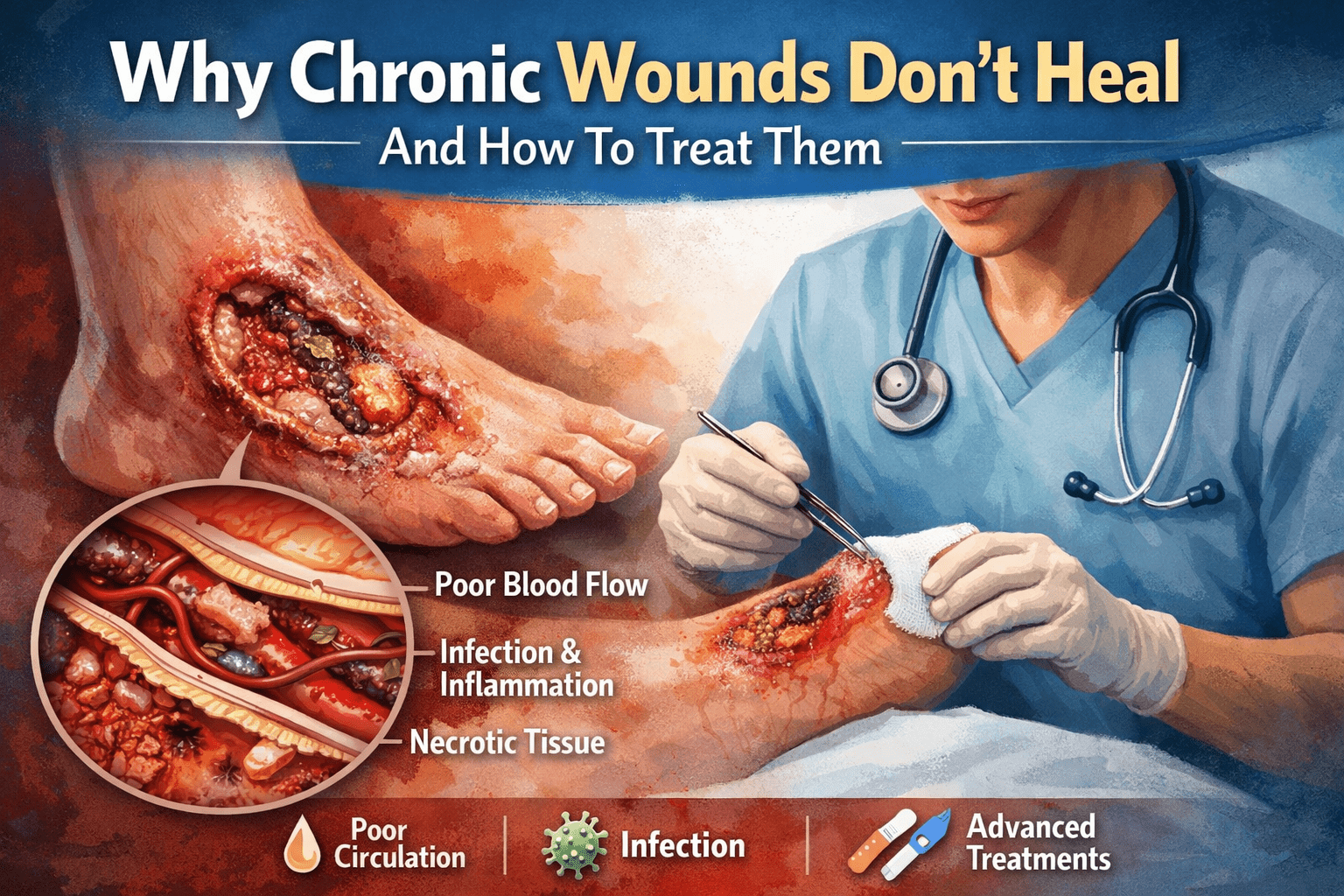
Medicare coverage questions often come up when a wound needs ongoing care, and getting to a clinic is difficult. For many people, pain, limited mobility, or a recent surgery can make frequent trips unsafe or unrealistic. Caregivers may also struggle to coordinate transportation, especially when appointments are needed several times per week. In those situations, understanding what Medicare will and will not pay for becomes an important part of planning care at home.
In this article, you’ll find out when Medicare may cover home wound care, what eligibility rules apply, and what costs to expect. You will also learn what is not covered, so you can plan your next steps with fewer surprises.

What counts as “home wound care”?
Home wound care usually means skilled nursing care provided in your home for a wound that needs clinical attention. For patients seeking mobile wound care in Ohio, this can include checking the wound’s size and condition, watching for infection, and choosing the right type of dressing based on drainage and healing progress. It may also include teaching a patient or caregiver how to protect the area and reduce pressure or friction that can slow healing. The goal is to keep the wound moving in the right direction while reducing complications.
Home wound care can apply to several wound types, including pressure injuries, surgical wounds, diabetic foot ulcers, burns, and other traumatic injuries, and chronic or non-healing wounds. Some wounds heal in a predictable timeframe, while others stall because of circulation problems, diabetes, limited mobility, or dead tissue that blocks healing.
Medicare focuses on whether the care is medically necessary and requires skilled clinical services, not just routine help. That distinction matters because it often determines whether care qualifies under home health benefits.
What are “home health services”?
When people ask whether Medicare covers home wound care, the key issue is whether it qualifies as Medicare home health services. Medicare may cover medically necessary, part-time or intermittent skilled nursing for wound care, such as treatment for pressure sores or surgical wounds, as long as the care is provided by a Medicare-certified home health agency.
It also helps to know what Medicare does not cover. Help with bathing, dressing, and other daily tasks is considered custodial care and is not covered when it is the only service needed. Medicare also does not cover 24-hour home care, meal delivery, or housekeeping that is not part of a medical care plan, so referrals and documentation must match the rules for skilled home health care.
Medicare Parts A, B, and C, and how each may apply to wound care
Medicare Part A usually applies when wound care is provided during a hospital stay or other inpatient care, where treatment is bundled into covered facility services. This often matters for Ohio patients who begin wound treatment in the hospital and then move into recovery at home.
Medicare Part B often applies to outpatient wound care and many home health-related services, including medically necessary treatment and certain supplies.
Medicare Part C (Medicare Advantage) must cover at least what Original Medicare covers, but plan rules can vary, including network limits and required approvals that may affect timing and out-of-pocket costs in Ohio.
Who qualifies for Medicare-covered home health wound care?
To qualify for Medicare-covered home health services, you usually must need part-time or intermittent skilled care, such as skilled nursing for wound treatment. Medicare generally limits combined skilled nursing and home health aide services to 8 hours per day, usually up to 28 hours per week (and up to 35 hours in certain cases). The care must be ordered as part of a medically justified plan.
You also must meet Medicare’s homebound rules. That means leaving home is difficult or not recommended, and you may need help from a device, special transportation, or another person. A provider must complete a face-to-face assessment before certifying home health services through the proper Medicare process.
What does Medicare cover?
When home wound care qualifies under Medicare home health rules, Medicare may pay for intermittent skilled nursing care. This can include wound assessment, dressing selection, dressing changes, and teaching that helps prevent complications such as infection or skin breakdown.
Medicare may also cover therapy services when they are part of the overall care plan, along with certain medical supplies used during treatment. In most cases, coverage centers on services that require clinical training and ongoing evaluation, which is why a clear care plan and consistent documentation support approval and continuity.
Medicare may also cover medically necessary wound dressings and related supplies. Primary dressings may include sterile gauze pads, hydrogel dressings, hydrocolloid dressings, and alginate dressings, while secondary supplies can include gauze wrap, bandages, and adhesive tape used to secure the dressing.
At the same time, Medicare generally does not cover 24-hour home care, meal delivery, or homemaker services like cleaning and shopping when they are not part of a medical care plan. It also does not cover custodial or personal care (such as bathing and dressing) when that is the only help needed, and it does not treat routine hygiene items the same way it treats medically necessary wound dressings, so families often need separate support for daily living needs.
Costs to expect
For many patients who qualify under the home health benefit, Medicare states that you pay $0 for covered home health services. That can include covered skilled nursing visits related to medically necessary wound care, as long as all eligibility and certification requirements are met.
This is one reason it is important to use a Medicare-certified home health agency and ensure the provider’s documentation supports the medical need. If coverage criteria are not met, the same services may be billed differently.
Costs can still come up for durable medical equipment (DME). Medicare notes that after you meet the Part B deductible, you generally pay 20% of the Medicare-approved amount for Medicare-covered medical equipment. For Medicare Advantage plans, your copays and cost-sharing can differ, even when the service is covered, and plan rules can affect which providers you can use.
In Ohio, checking whether a provider is in-network and whether approvals are required can help you avoid unexpected bills tied to plan policies.
Is Medicare coverage different in Ohio?
Medicare is a federal program, so the core coverage rules for home health and wound care do not change from state to state. That means the same homebound standards, skilled need requirements, and certification rules apply in Ohio just as they do elsewhere.
What can feel “different” in Ohio is not the Medicare rulebook, but how care is accessed and delivered in your area. Provider availability and care coordination steps can shape how quickly services begin.
Local factors can include which home health agencies serve your county, how fast a referral can be processed, and whether a mobile wound care provider can travel to your home or care setting.
If you have Medicare Advantage, network rules can matter more than location, since your plan may limit which agencies and clinicians you can use. The practical takeaway is that patients in Ohio should confirm both Medicare eligibility and local provider access at the same time. That combination helps prevent delays that can worsen a wound.
Getting started: Step-by-step checklist
Getting started usually begins with your primary care provider, specialist, or hospital discharge team. A provider must order the services, and a qualified clinician must assess you face-to-face before home health services are certified.
If home wound care is needed, your provider can document why skilled care is necessary and whether you meet the homebound standard. Strong documentation supports faster coordination and fewer coverage disputes.
It also helps to clarify your Medicare coverage type before scheduling begins. If you are on Original Medicare, confirm the agency is Medicare-certified and understands home health billing rules.
If you are on Medicare Advantage, confirm the provider is in-network and ask whether prior approval is required.
You should also ask how wound supplies will be handled, including which supplies are covered and how replacement timing is determined under the care plan.
Conclusion
In many cases, Medicare does cover home wound care as long as the care qualifies under Medicare’s home health services rules, including a skilled need, homebound status, and proper provider certification. When coverage applies, Medicare notes that patients pay $0 for covered home health services, while DME may involve Part B cost-sharing.
At Inspiring Minds Wound Care in Ohio, we see to it that patients and families understand the care plan details, the coverage process, and eligibility requirements, so treatment can begin without unnecessary delays. The most practical path is to secure a clear referral, confirm eligibility, and verify provider and plan requirements so wound care starts on time and stays consistent.